Potty Training – How to Get the Job Done!
June 6, 2022
Back to School Eye Health Tips
August 3, 2022What temperature constitutes a “fever”?
A fever occurs when there is an above-normal increase in the body’s temperature. Although body temperatures fluctuate from person to person, most medical professionals agree that a temperature of 100.4˚ Fahrenheit or higher would be considered a fever, especially for a young child.
Why do fevers occur?
There is a multitude of reasons why a fever may occur. Frequently, fevers signify that the body may be fighting an infection. A fever may also occur after receiving a vaccine or overheating from heat exhaustion or sunburn. Fevers, in many cases, will go away on their own and do not have to be treated; however, fevers in children can be highly dangerous if not observed. Be sure to keep a close eye on your children if you notice that they have spiked a fever. Please continue reading for important information on how to combat your child’s fever and when to know it is time to see a doctor.
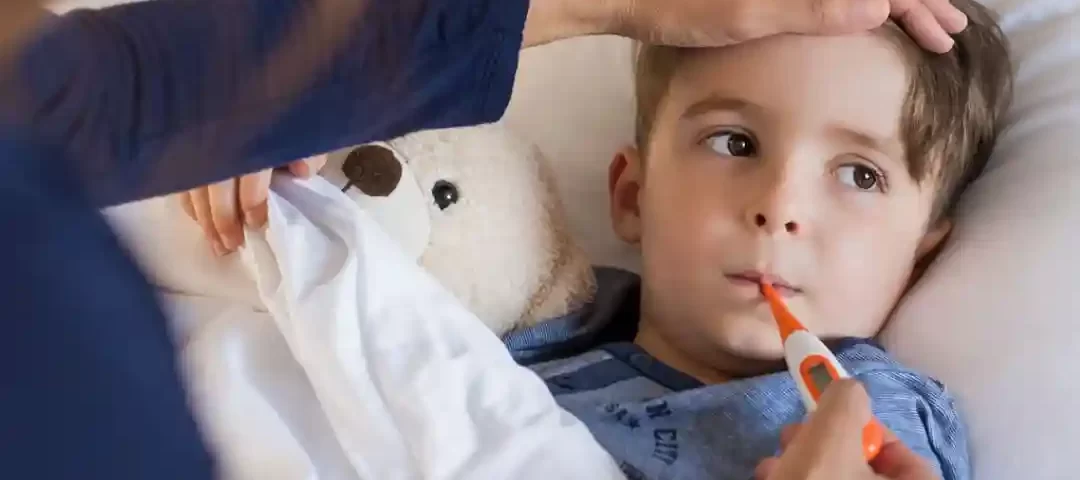
How to take a child’s temperature?
There are several ways to take a child’s temperature! If you notice that your child is a little warmer than usual, whether they are showing symptoms of a cold or not, you can take their temperature with a:
- Rectal thermometer – This thermometer is inserted into the rectum (baby’s bottom). Rectal thermometers are one of the most accurate ways to get a body temperature.
- Forehead thermometer – If used correctly, forehead thermometers can accurately read a baby’s temperature.
- Oral (mouth) thermometer – Oral thermometers are placed in the mouth, under the tongue. If you use this thermometer on your child, be sure to wait 30 minutes after they have consumed anything hot or cold.
- Tympanic (ear) thermometer – When using an ear thermometer on your child, be sure to wait 15 minutes if they have been exposed to a cold environment.
- Axillary (armpit) thermometer – Arguably one of the least accurate ways to check for a temperature; however, it can be used for a quick check if it is the only thermometer available at the time.
Checking temperatures accurately for their age:
- Four months and under: Both rectal and forehead thermometers are a good choice.
- Five months and under: Rectal, forehead, and axillary thermometers can be used effectively.
- Six months and over: Rectal, forehead, and axillary thermometers can be used effectively.
- Four years and older: Tympanic (ear), oral, forehead, and axillary thermometers are good choices.
Always inform your child’s pediatrician of the method of temperature checking you are using with your child.
How to know it’s time to see the doctor!
Never hesitate to contact your child’s pediatrician if you have concerns regarding your child’s health. If your child is experiencing any of the following, you should call their health care provider right away:
- If they are under three months old and, have a temperature of 100.4˚F or higher.
- If they are over three months old and have a temperature of:
- 104˚F or higher
- 102˚F or higher for over two days and will not come down, even after being given treatment.
- Has a fever at any age, and:
- If they get a rash.
- If they Do not have an appetite and are showing signs of dehydration.
- If their urine is dark.
- Have a stiff neck, headaches, or sharp pains in the stomach.
- If they are fatigued and look pale.
- Have health conditions that may compromise their immune system, such as; cancer, sickle cell, etc.
If you suspect your child is experiencing a medical emergency, contact 911 immediately. At SuraMed Health Center, we are passionate about giving children the quality care they deserve. To learn more about our services, please visit our website today.